Baseline characteristics
2,922 individuals over 60 years old with GNRI score were selected for analysis, among whom 2,670 (91.37%) had high GNRI (≥ 98) and 252 (8.63%) had low GNRI (< 98). Participants in low GNRI group were significantly older than higher GNRI group (mean age: 73.56 ± 7.91 vs. 71.62 ± 7.30 years, P < 0.001), but with no significant difference shown on sex and race distributions (P = 0.875 and P = 0.347). Individuals with low GNRI exhibited an increased prevalence on having lower education levels or being widowed, divorced, or separated (all P < 0.01). Additionally, low GNRI participants tended to have lower PIR (P = 0.014). Regarding lifestyle factors, alcohol consumption and BMI distribution varied significantly across groups (both P < 0.001). More participants with low GNRI were never drinkers (47.22% vs. 55.51%) and had BMI < 25 kg/m² (30.95% vs. 20.94%). However, a large percentage of BMI data was missing in the low GNRI group (28.57% vs. 0.79%). Moreover, comorbidity analysis revealed a higher prevalence of stroke (13.89% vs. 7.68%, P < 0.001) and cardiovascular disease (37.70% vs. 26.59%, p < 0.001) in the low GNRI group. But a notably reduced prevalence of hyperlipidemia (58.17% vs. 85.54%, P < 0.001) was indicated as well. Nevertheless, no significant differences have been presented in hypertension, diabetes, or Parkinson’s disease among different GNRI levels (Table 1).
Correlation between GNRI and mortality
When treated as a continuous variable, higher GNRI levels were associated with decreased risk of all-cause mortality in all three models (Model 1: HR = 0.987, 95% CI: 0.984–0.989, Model 2: HR = 0.991, 95% CI: 0.988–0.993, Model 3: HR = 0.993, 95% CI: 0.990–0.996, all P < 0.001). Similarly, higher GNRI scores were also linked to decreased risk of cardiovascular mortality in Model 1 (HR = 0.986, 95% CI: 0.982–0.990, P < 0.001), Model 2 (HR = 0.999, 95% CI: 0.987–0.995, P < 0.001) and Model 3 (HR = 0.991, 95% CI: 0.986–0.997, all P = 0.002). As a categorical variable, higher GNRI (≥ 98) was also correlated with decreased risk of all-cause mortality, with HR of 0.492, 0.528, and 0.669 in the Model 1 (95% CI: 0.415–0.583, P < 0.001), 2 (95% CI: 0.444–0.628, P < 0.001) and 3 (95% CI: 0.543–0.823, P < 0.001), respectively. For cardiovascular mortality, high GNRI was also observed as protective factor, with HR of 0.455, 0.509, and 0.592 across the respective models (Model 1: 95% CI: 0.342–0.605, P < 0.001, Model 2: 95% CI: 0.380–0.681, P < 0.001, Model 3: 95% CI: 0.418–0.838, all P = 0.003) (Fig. 2). Similarly, consistent results have been presented in participants who excluded missing values (Table S1). Furthermore, our results were validated by survival analysis (Fig. 3). Specifically, participants in the higher GNRI group had lower all-cause and cardiovascular survival rates (both P < 0.001). Schoenfeld residual analysis did not find any violating assumptions (all P > 0.05), nor did it identify any collinearity issues (variance inflation factor < 5) (Figure S1). According to RCS analyses, the correlation of all-cause mortality was nonlinear (P = 0.001), and the J-shaped curve has been shown in Fig. 4 with the lowest point at GNRI = 120. Also, a similar J-shaped association was also observed for cardiovascular mortality (P for non-linearity = 0.04). Moreover, the overall associations were statistically significant (P for trend < 0.001 and 0.008). To ensure the robustness of the findings, sensitivity analyses excluding GNRI values above 180 and 190 were conducted separately, and the non-linear association remained significant (Figure S2).

Correlation between GNRI and all-cause mortality and cardiovascular mortality in OA
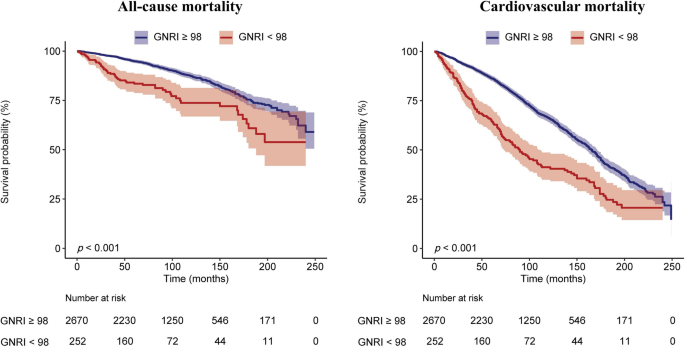
Kaplan Meier survival rates of all-cause mortality and cardiovascular disease in different GNRI groups of OA patients
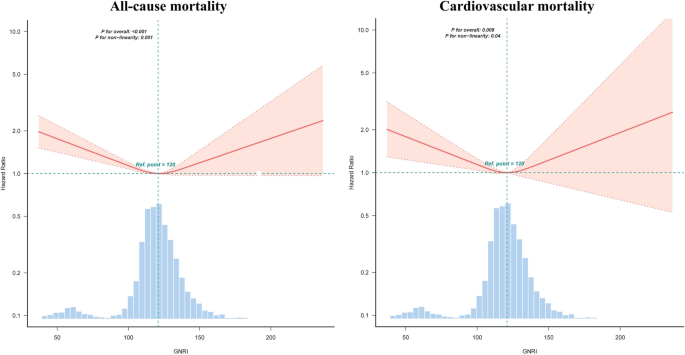
Restricted cubic spline regression of GNRI and cardiovascular mortality and all-cause mortality in OA patients. Adjusted demographic characteristics, lifestyle factors, and health status
Nonlinear and threshold effect analysis
RCS and piecewise regression analyses demonstrated a nonlinear correlation between GNRI and mortality, with a consistent inflection point at GNRI = 120. For all-cause mortality, there was a significant negatively connection in the linear model (Model 1), which remained in Model 2 when GNRI < 120. Interestingly, a slightly increased risk was observed when individuals of GNRI ≥ 120 were included (HR = 1.011, 95% CI: 1.002–1.019, P = 0.018). The log-likelihood ratio test favored the piecewise model over the linear one (P = 0.001), indicating a significant threshold effect. For cardiovascular mortality, similar trends were observed. In summary, the linear model showed an inverse association of both all-cause and cardiovascular mortality. In the piecewise model, the association was significant when GNRI was below 120, which became insignificant above this threshold (HR = 1.008, 95% CI: 0.995–1.020, P = 0.230). The log-likelihood ratio test also supported the nonlinear model, with details shown in Table 2 (P = 0.040).
Subgroup analyses
Subgroup analyses have been carried out to shed light on the potential correlation of GNRI categories and both mortality among diverse demographic and clinical features. The associations remained generally consistent across subgroups, with no statistically significant interactions observed.
For all-cause mortality, low GNRI score (< 98) exhibited significantly higher HR compared to those with higher GNRI (≥ 98) in most subgroups. And it was validated in both subgroups determined by age (< 70 or ≥ 70). Moreover, compared with the group with higher GNRI, males with lower GNRI (HR = 2.009, 95% CI: 1.445–2.792, P < 0.001) had a much higher risk than females (HR = 1.435, 95% CI: 1.102–1.869, P = 0.007). Across racial subgroups, the association was most pronounced in non-Hispanic Whites (HR = 2.062, 95% CI: 1.632–2.606, P < 0.001). In addition, participants with higher education levels and income also exhibited significantly increased risks with lower GNRI. Similar trends were seen across smoking status, alcohol consumption, and BMI subgroups, with notably higher risks observed in never smokers (HR = 1.628, 95% CI: 1.178–2.250, P = 0.003) and never drinkers (HR = 1.625, 95% CI: 1.199–2.202, P = 0.002). Lower GNRI was also associated with higher mortality among individuals without hypertension (HR = 2.918, 95% CI: 1.803–4.721, P < 0.001) and without hyperlipidemia (HR = 1.470, 95% CI: 1.050–2.057, P = 0.025). All the details of subgroup analysis related to all-cause mortality could be seen in Fig. 5.

The correlation between all-cause mortality and cardiovascular disease in subgroups of OA patients with GNRI. PIR, Poverty Income Ratio; BMI, Body mass index
For cardiovascular mortality, similar associations were observed in both age groups, compared with females (HR = 1.618, 95% CI = 1.027–2.550, P = 0.038), males have a significantly higher risk with lower GNRI levels (HR = 2.934, 95% CI: 1.743–4.939, P < 0.001). Similarly, the association was the strongest in non-Hispanic Whites (HR = 2.406, 95% CI: 1.639–3.532, P < 0.001) among all racial groups. Additionally, significantly increased cardiovascular mortality risk with low GNRI was also presented among participants with college education (HR = 1.782, 95% CI: 1.009–3.147, P = 0.047), higher income (PIR > 3.5; HR = 2.527, 95% CI: 1.038–6.153, P = 0.041), and never drinkers (HR = 2.672, 95% CI: 1.425–5.009, P = 0.002). Furthermore, elevated risk was further observed in those without hypertension (HR = 4.921, 95% CI: 2.116–11.443, P < 0.001), without hyperlipidemia (HR = 2.188, 95% CI: 1.244–3.849, P = 0.007), and without cardiovascular disease (HR = 1.499, 95% CI: 1.219–1.844, P < 0.001). Details of subgroup analysis on cardiovascular mortality could be found in Fig. 5.
Notably, no significant interaction was found between GNRI and any of the subgroup variables for either all-cause or cardiovascular mortality (P for interaction > 0.05 for all), suggesting that the impact of low GNRI on mortality was consistent across different strata.
link

