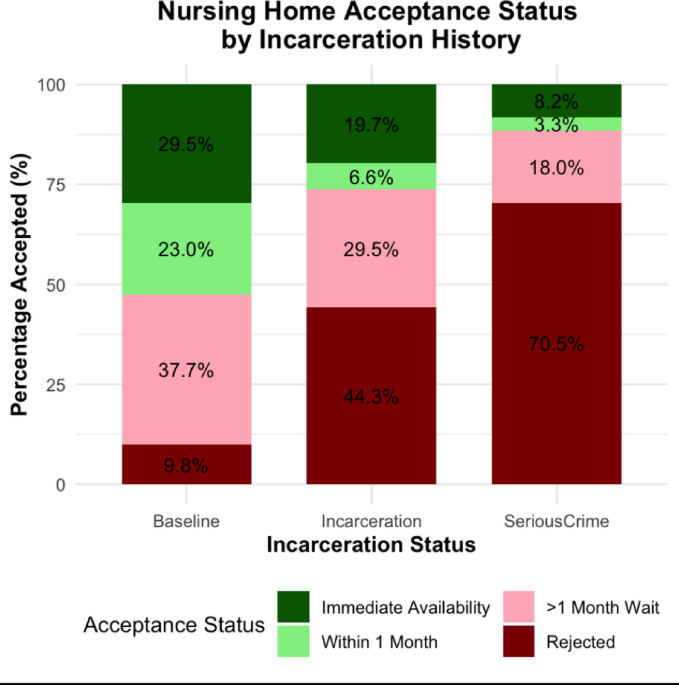
This study sought to explore the impact of incarceration and compassionate release status on the availability of nursing home placement, and the associated perceived barriers to admissions. At baseline, the majority of RI nursing homes reported bed availability within 1 month. A significant group of facilities did have long waitlists, suggesting that long-term nursing care is a limited resource for any person coming from the community. However, while a substantial number of admissions coordinators endorsed extended waitlists longer than 1 month, very few nursing facilities outright rejected patients during the initial survey of bed availability.
The disclosure of incarceration and compassionate release status dramatically influenced the possibility of nursing home placement, with many admissions coordinators changing their responses to rejection. After discovering the incarceration status of the prospective patient, bed availability within 1 month was cut in half. Furthermore, a large number of facilities (41%) stated that incarceration may impact admissions but did not deliver a definitive answer. As a result, our results are likely conservative estimate. Only 4 facilities (6.6% of all nursing homes) endorsed bed availability within 1 month without qualifying that incarceration might impact admissions. In summary, while some nursing homes were willing to consider compassionate release patients for admission, most facilities either rejected incarcerated patients despite existing bed availability or expressed concern about incarceration status without explicit rejection.
Violent offenses and other serious crimes had a particularly pronounced impact on nursing home admissions, with facilities more likely to deny admissions to those with serious offenses on their criminal record. The bulk of admissions coordinators explicitly stated they would not accept an incarcerated patient with a “serious offense” on their record for nursing home admissions, and nearly 90% of nursing homes in RI were unavailable to incarcerated patients with a “serious offense” on their record.
Many people eligible for medical parole many have had long incarcerations. As most incarcerated persons in RI who are serving sentences greater than 10 years have committed violent or other serious crimes, these data suggest that nursing home placement is virtually non-existent for most compassionate release candidates15. Thus, the population most eligible for compassionate release may also be the population least likely to be accepted by nursing homes.
Specific concerns regarding patient safety, care complexity, and institutional policies were commonly cited by admissions coordinators as barriers to accepting individuals granted compassionate release. Notably, multiple respondents described the patient as “too complex,” despite the standardized model profile having relatively low medical acuity. Nearly a quarter of facilities explicitly cited incarceration itself as the primary barrier to admission, suggesting that criminal legal history—not clinical need—often drove exclusion.
These concerns may reflect stigma more than evidence. Compassionate release is often contingent on a thorough review by parole boards, which explicitly assess public safety risk prior to approval. Moreover, empirical data demonstrate that individuals over the age of 55 have extremely low recidivism rates of 0.2–0.4%16.
Despite the evidence of decreased recidivism among older incarcerated people, admission coordinators’ responses regarding safety, complex patient needs, and behavioral challenges highlight that nursing homes may feel ill-equipped to care for patients with a history of incarceration. Resident-to-resident and resident-to-staff physical violence are both known entities in nursing homes. However, neither have been systematically correlated with prior criminal offenses and are, instead, associated with cognitive impairment among residents and staffing constraints17,18,19. This further highlights how criminal legal stigma may be influencing health decision-making.
Criminal legal stigma has been repeatedly demonstrated to negatively impact the housing and health of justice-involved individuals’ post-incarceration20,21.
As it stands, incarcerated persons are not explicitly protected under the Fair Housing Act, allowing for a history of incarceration to remain a legal and legitimate reason for a housing provider to reject an applicant22. Provided that the FHA has been shown to apply to nursing homes23,24, nursing facilities can selectively exercise bias and reject applicants due to their incarceration status. However, since incarcerated people are disproportionately members of racial and ethnic classes that are protected under the FHA, the United States Department of Housing and Urban Development issued a 2016 guidance on the “Application of Fair Housing Act Standards to the Use of Criminal Records.” This guidance clarifies that, while a nursing home, for example, may reasonably consider criminal legal involvement as a factor for denying admission if it aligns with the facility’s interests and needs, generalized or arbitrary criminal history-based restrictions are likely to discriminate against protected groups, thereby potentially violating the FHA22. As such, the FHA may offer a potential pathway to challenge blanket exclusions based on incarceration, particularly when such practices disproportionately impact marginalized groups protected by the FHA.
Admissions coordinators’ perceived barriers to accepting a compassionate release patient may stem from the cost-benefit analysis that must be conducted on every prospective admission. Since insufficient Medicaid reimbursements often force nursing homes to operate on thin or negative margins, nursing facilities must always consider if the resource utilization from accepting and caring for a patient is worth the reimbursement25,26. Therefore, even a perceived risk of increased liability that a history of incarceration may carry has the potential to swing that cost-benefit analysis toward denying admission to justice-involved patients27.
These perceived barriers, paired with our quantitative findings of significantly limited bed availability for incarcerated patients, suggest that alternative nursing home placement options are required for older incarcerated individuals granted compassionate release to receive the care they need.
This is the first study to examine the real-world availability of community nursing home services for incarcerated persons seeking compassionate release. Our findings suggest that the limited state-wide availability of nursing home care to incarcerated individuals is a barrier to the widespread implementation of compassionate release laws. If this policy and market gap is not addressed, patients may continue to remain incarcerated and unable to receive more appropriate nursing care as they age or illness advances.
Limitations
These findings may underestimate the number of nursing homes that would reject patients coming from carceral settings. The way questions were posed regarding incarceration status and criminal history may have introduced the social desirability bias28. Put differently, the study design could not prevent admissions coordinators from saying they would still consider an incarcerated patient for nursing home admissions because that is the socially desirable response when, in reality, the patient would be rejected later in the process for unspecified reasons.
Another limitation of this study is that it primarily quantified the responses of nursing home admissions coordinators. While we can assume that the responses of admissions coordinators reflected the official policies of the long-term nursing facilities themselves, there may be some discrepancy between responses during a brief phone call and the official nursing facility policy, and likewise between policy and practice. However, admissions coordinators are the primary point of contact for individuals seeking long-term nursing care, and so this may reflect real-world dynamics more accurately.
This study is further limited by generalizability. While 82.4% of long-term nursing facilities in Rhode Island were successfully included, Rhode Island is a uniquely small state with no state-run public nursing home. As such, the specific nursing home landscape in Rhode Island may not translate to other states that may be better equipped to provide nursing home care to incarcerated patients granted compassionate release.
The problem of generalizability also applies to how much of a challenge the compassionate release process is in RI compared to other states. A 2018 study by Families Against Mandatory Minimums (FAMM) assigned a report card for every state’s compassionate release programs. RI is 1 of 5 states that received an A, A+, or A- grade, compared to 34 out of 50 states that received an F29,30. Since one of the metrics the FAMM study judged compassionate release programs on was the efficacy of discharge planning, it is possible that the results of this study may be more dramatic in many other states.
The model patient used in our study had a specific set of characteristics that may not be reflected in real-world incarcerated persons granted compassionate release. Other medical conditions or criminal legal system factors may increase or decrease the likelihood of placement. Our sample patient was stated to be able to pay privately for nursing home care for 1 year. This was done to eliminate insurance as a factor for bed availability to truly isolate incarceration as the sole independent variable impacting responses in this study. However, the reality is that most incarcerated patients cannot privately pay for long term nursing care and would likely rely on Medicaid31. Nursing homes frequently have limited Medicaid beds, creating a separate financial barrier to nursing home admissions from the community32. Incarcerated patients granted compassionate release may, therefore, face other barriers to finding a nursing home bed beyond incarceration itself.
Facility size was assessed as a potential confounder, though it did not significantly impact results. However, other unmeasured facility-level factors such as ownership status, staffing capacity, or proximity to schools (in cases of a sexual offense) could also influence decision-making and warrant future study.
link