Osteoarthritis (OA) is a prevalent chronic degenerative disease and a leading cause of disability in elderly individuals. The knee joint is the most commonly affected site of OA15. KOA accounts for approximately four-fifths of the global OA burden, with its incidence increasing alongside obesity and aging16. In the early stages, KOA primarily manifests as knee pain and tenderness, often aggravated by descending stairs or vigorous activities. In advanced stages, it can result in restricted joint mobility, muscle atrophy, physical disability, and diminished quality of life17. While KOA remains incurable, total knee arthroplasty (TKA) is considered an effective treatment for late-stage disease, albeit associated with substantial healthcare costs18. Consequently, significant research attention has shifted toward the prevention and treatment of early-stage KOA19. Pain management and the prevention of KOA progression are key therapeutic goals20.
Several studies have identified risk factors for KOA progression, including female sex, age ≥ 40 years, overweight or obesity, and a history of knee joint trauma. Protective factors include engaging in physical activity and having a higher level of education (e.g., high school or college)5,21. However, factors such as age and sex are non-modifiable through home-based management or healthcare interventions. Advances in KOA-related research have underscored the importance of identifying modifiable risk factors and exploring protective factors to delay or prevent KOA onset, ultimately alleviating the societal burden associated with the disease. According to the 2019 guidelines issued by the American College of Rheumatology (ACR) and Arthritis Foundation, knee joint injuries and excess body weight are preventable risk factors that can be managed at home12. Thus, it is strongly recommended that patients control their weight at home to prevent the onset and progression of KOA. Previous study found that higher educational attainment is associated with a reduced risk of KOA, potentially due to the reduced physical labor and lower risk of knee joint injury associated with advanced education22. Furthermore, the 2019 OARSI guidelines recommend exercise as a preventive measure for KOA18. However, the 2019 ACR guidelines strongly advocate for physical activity as a protective factor for KOA prevention, while emphasizing the need for further research to determine specific exercise types that effectively protect the knee joint12. Some scholars have noted that moderate exercise can help prevent KOA, whereas excessive exercise may increase its risk23. Therefore, further research is needed to establish an optimal exercise regimen for KOA prevention.
One factor that directly influences KOA progression, prognosis, and patients’ quality of life is joint deformity. Flexion deformities typically stem from soft tissue pathologies, while varus and valgus deformities are more frequently caused by bony abnormalities. Many patients develop knee flexion contracture during the disease course, which limits the passive range of motion in the affected knee joint24. Reduced lower-limb joint mobility restricts physical activity, exacerbates pain and stiffness, and may interfere with basic daily activities such as standing and walking25,26. Flexion contracture not only impairs mobility but also increases energy expenditure, the risk of falls, and wear on adjacent joints such as the hip and lumbar spine24,27. From a biomechanical perspective, flexion contracture limits the weight-bearing surface of cartilage, concentrating mechanical stress on smaller joint areas28. In cases with pre-existing cartilage damage, localized tissue swelling and flexion contracture may accelerate cartilage degeneration, leading to chondrocyte apoptosis and further cartilage deterioration29. Besides KL grade, other factors such as knee effusion, pain intensity, disease duration, and age are recognized risk factors for joint replacement30,31. Notably, 33–80% of patients undergoing TKA present with knee flexion contracture deformities, highlighting the close relationship between deformities and TKA32. Flexion contracture may reduce the overall contact area of the articular surface, impairing the load-bearing function of relatively healthy cartilage or subchondral bone, thereby intensifying OA-related pain33. Conversely, pain can lead to loss of mobility as patients restrict knee joint movement to avoid painful weight-bearing postures (e.g., full knee extension), perpetuating and worsening flexion contracture over time. In this context, loss of knee joint mobility and knee pain may create a synergistic negative cycle. A cohort study demonstrated that early intervention for flexion contracture could help reduce the incidence of knee OA, slow radiographic progression, and delay the need for TKA6.
The findings of this study reveal a prevalence of approximately 36.11% for knee flexion contracture among patients with KOA, with a higher proportion observed in women and older individuals, consistent with known KOA risk factors. Patients with flexion contracture were also characterized by longer disease duration and higher KL grades, suggesting that joint deformity is a common late-stage complication of KOA and a significant contributor to disability. However, joint deformities were also identified in patients with shorter disease durations and lower KL grades (I-II), indicating that deformities can arise at any stage of the disease. Adjacent joint misalignment, particularly of the hip and ankle, plays a crucial role in the pathogenesis and progression of knee deformities. Studies have demonstrated that hip flexion contracture or ankle equinus can alter lower limb biomechanics, leading to increased stress on the knee joint and exacerbating flexion contracture34,35. Specifically, Alireza Mirahmadi34 highlighted that hip abduction-adduction imbalance correlates with knee valgus deformity, while Zainb Al-Bayati35 reported that ankle dorsiflexion restriction contributes to compensatory knee flexion during gait. These findings emphasize the need to consider multi-joint interactions in understanding knee osteoarthritis-related deformities.
Prior research has suggested that joint deformities are critical factors in KOA progression6,36. Joint deformities and the degenerative changes associated with KOA have a bidirectional and mutually reinforcing relationship; without timely intervention, the disease may progress into a detrimental cycle33. The knee joint, as the body’s primary weight-bearing joint, is particularly susceptible to the effects of obesity, which increases joint load, thereby exacerbating cartilage damage, subchondral fractures, and articular collapse, ultimately resulting in deformities. Tran DH37 reported that weight reduction alleviates pain symptoms and improves knee joint mobility. Additionally, joint injuries may cause cartilage damage and associated inflammatory responses, which accelerate cartilage deterioration38. A history of osteoporosis is also linked to joint deformities, while regular use of calcium supplements has been shown to reduce the incidence of deformities, suggesting a possible association with bone metabolism. Occupational factors, such as manual labor, prolonged standing, walking-intensive commuting, living in high-rise buildings without elevators, using squatting toilets, and frequent hiking, can exacerbate knee joint stress. Prolonged overloading can worsen cartilage and subchondral bone damage. Conversely, regular knee joint exercises strengthen joint stability through the targeted training of muscles such as the popliteus, gastrocnemius, and quadriceps, which helps reduce muscle fatigue, prevent spasms, and lower the risk of deformities39. Patients with KOA with joint deformities exhibited higher VAS scores, indicating greater disease severity and a more urgent need for pain management. Furthermore, higher WOMAC total scores, as well as sub-scores for pain, stiffness, and function, in the deformity group underscore the detrimental impact of joint deformities on mobility, local inflammation, and overall quality of life.
The study highlights significant risk factors for knee flexion contracture among patients with KOA, such as older age, female sex, higher BMI, a history of knee trauma, and higher KL grades. These findings emphasize the importance of early identification and targeted management of high-risk individuals to prevent or slow the progression of flexion contracture. Modifiable factors like physical activity, calcium supplementation, and reducing occupational and lifestyle-related joint stress (e.g., avoiding squatting postures and excessive stair climbing) can be addressed through patient education and personalized interventions. This underscores the need for tailored prevention strategies to reduce the prevalence of flexion contracture. The protective effect of regular knee exercises calls for incorporating structured exercise programs into the rehabilitation plans of KOA patients. Emphasis should be placed on identifying optimal exercise regimens to strengthen joint-supporting muscles and improve joint stability. With flexion contracture affecting over one-third of KOA patients, public health initiatives should focus on raising awareness of risk and protective factors, promoting weight management, and improving access to preventive care and physical therapy services.
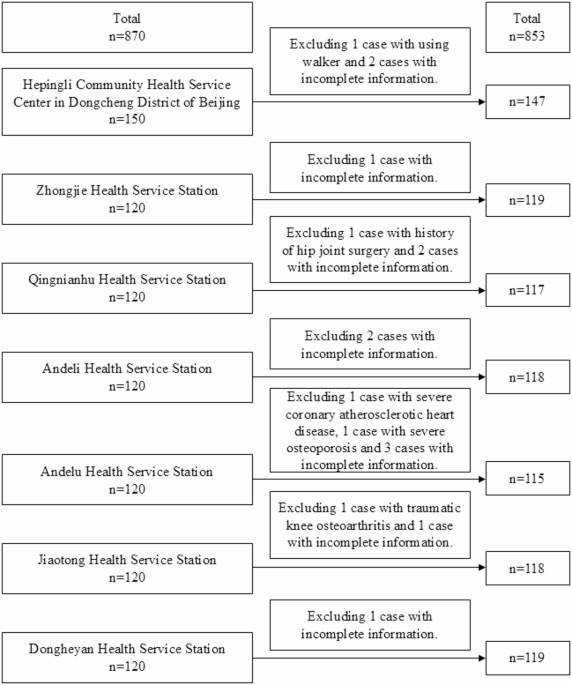
Our study has several limitations that must be considered. Firstly, this study is a cross-sectional study, which can only reveal associations but cannot establish causality. Future research should employ longitudinal studies or interventional trials to further explore causal relationships. Secondly, the study sample was collected exclusively from seven community hospitals in Beijing, China, which may limit the generalizability of the findings. This is particularly relevant for patients with KOA in other regions or different healthcare institutions. Thirdly, this study did not investigate medical diseases such as coronary heart disease, hypertension, diabetes, and metabolic syndrome, which limited the exploration of the internal mechanism of joint deformity. Additionally, we did not evaluate the alignment of adjacent joints (e.g., hip and ankle) or their potential influence on knee flexion contracture. There may also be recall bias towards variables such as trauma history and lifestyle habits. Finally, although exercise was identified as a protective factor, the study did not provide detailed insights into which types or intensities of exercise are most effective, highlighting the need for more refined data collection in this area.
link