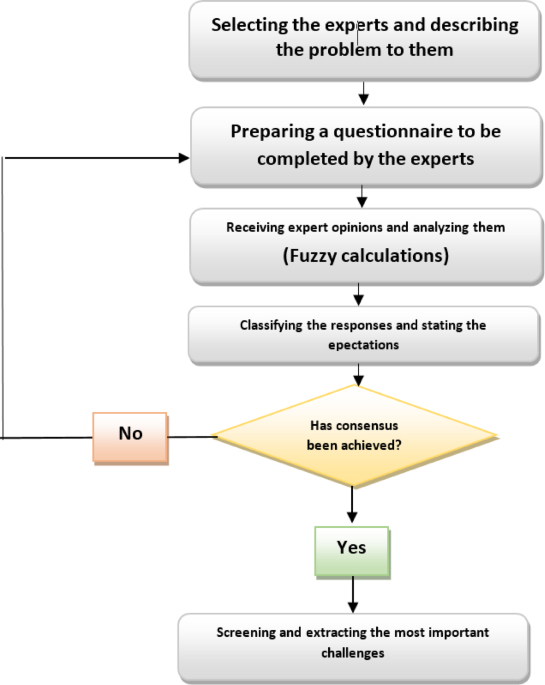
This study aimed to explore the challenges of geriatric health care services (GHCSs) in Iran using qualitative methods. The findings indicate that Iran’s health system faces multiple challenges in providing GHCS, including issues related to education, infrastructure, workforce, financing, supervision, elderly-specific problems, and service delivery. A key contribution of this study is its comprehensive identification of practical barriers in Iran’s GHCS system, based on firsthand insights from diverse stakeholders. What makes these findings innovative is the integrated understanding they provide of how fragmented policies, weak institutional accountability, and limited geriatric infrastructure collectively create systemic barriers to elderly care.
These challenges, while specific in their local manifestations, reflect broader patterns observed in other middle-income countries. For instance, the issue of fragmented intersectoral collaboration—such as poor coordination between the Ministry of Health and the State Welfare Organization in Iran—is also reported in countries like Brazil and South Africa, where overlapping responsibilities among health and social welfare institutions hinder integrated elder care31,32. Similarly, insufficient insurance coverage and unequal access to services are shared concerns across many developing countries, including India and Indonesia, where elderly populations face high out-of-pocket costs and limited geriatric infrastructure33,34. However, what sets Iran apart is the existence of a National Policy Document on Ageing (NPDA) that remains largely unimplemented, whereas some peer countries have begun operationalizing national aging strategies through dedicated agencies and better policy enforcement35,36.
Based on interview data and FDM/FMEA analyses, 18 key challenges were identified and are described below.
Lack of health insurance coverage for old age groups
One of the main challenges identified in this study is inadequate insurance coverage for the elderly. Studies show that poverty and economic dependence in old age limit access to healthcare and increase the risk of catastrophic health expenditure37,38,39. Inadequate coverage of essential services like rehabilitation and failure to protect households financially are also noted concerns21,22,23,24. Additionally, the high prevalence of chronic diseases among the elderly strains insurance systems, as these predictable conditions are not aligned with traditional insurance models designed for unexpected risks40. Given these issues, experts stress the need for targeted insurance programs to support the elderly’s physical, emotional, and financial well-being. Policymakers are encouraged to design and implement strategies to enhance insurance and support coverage for this population group. However, several barriers may hinder the successful implementation of such policies. These include limited financial resources and competing health priorities at the national level, administrative inefficiencies in insurance organizations, and lack of intersectoral coordination between health, social welfare, and insurance agencies. Additionally, resistance to policy reform, particularly in systems with entrenched bureaucratic structures, can delay or dilute the intended impact. Addressing these obstacles requires strong political commitment, stakeholder engagement, and phased implementation strategies tailored to local contexts.
Existence of parallel and unprofessional public agencies and lack of coordination between MOHME and SWO
A key challenge identified in GHCSs is the presence of parallel and unprofessional public agencies and poor coordination between MOHME and SWO. Studies have noted contradictions between responsible ministries and overlapping, uncoordinated agencies involved in elderly care37,41. This situation leads to conflicting decisions, wasted resources, and increased costs for the health system, service providers, and recipients. This issue refers to the operational fragmentation between existing actors and the lack of streamlined service protocols. The lack of inter-organizational coordination and policy integration further results in inefficient resource allocation and service overlap. Hence, to address the issue of fragmented governance and lack of coordination between MOHME and SWO, establish a legally mandated “National Elderly Care Coordination Council” co-chaired by MOHME and SWO, with representatives from other key ministries (e.g., Interior, Welfare, and Labor). This council should have clearly defined roles, a dedicated budget, and authority to align programs, streamline service delivery, and prevent duplication. Moreover, develop a joint annual action plan and create a unified monitoring and evaluation system to ensure accountability and policy coherence. However, several barriers may impede the implementation of these coordination mechanisms. Institutional resistance to change, unclear jurisdictional boundaries, and competition over leadership and budget control between agencies may delay or weaken inter-organizational collaboration. Additionally, the absence of a strong legal framework and enforcement mechanisms could result in limited compliance with council directives. Limited technical capacity and insufficient data sharing infrastructure may also challenge the development of an integrated monitoring system. Addressing these obstacles requires strong political leadership, clear legislative backing, capacity-building efforts, and an inclusive approach that fosters trust and cooperation among stakeholders.
Inadequate budget allocation for GHCS provision
Another major challenge identified was insufficient financial support and the low budget share allocated to the geriatric health sector. Samouei et al.42 noted the threat of inadequate GHCS financing to the Iranian health system, and Karami Matin et al.43 reported that elderly healthcare costs are nearly five times higher than for other groups. A potential policy approach could involve allocating a dedicated budget line for geriatric health services based on population needs, alongside introducing performance-based financing to enhance service quality and efficiency. However, the implementation of such financial reforms may face several barriers. These include limited fiscal space within national and provincial health budgets, competing priorities that favor curative over preventive or long-term care services, and weak political will to prioritize aging-related health needs. Moreover, the lack of reliable data on geriatric service utilization and outcomes can hinder the development of effective performance-based financing mechanisms. Bureaucratic inertia and fragmented financial planning between sectors may also delay budget realignment. To overcome these challenges, strong advocacy, evidence-informed budgeting, and pilot programs demonstrating cost-effectiveness and impact may be required to build momentum for sustained investment in GHCSs.
Lack of legislation on intersectoral collaboration between hospitals and geriatric day care centers
In line with this part of the findings, other studies have also underlined the lack of a link between different levels from prevention to rehabilitation, the lack of palliative and end-of-life care, and disregard for annual check-up programs for the elderly as geriatric care challenges37,41,44,45. This lack of integration between different levels of services can lead to the elderly’s confusion among different offices, receiving different treatments, and inadequate treatment follow-up46. A policy recommendation to address the lack of legislation on intersectoral collaboration is to draft and implement a national guideline that mandates integrated care pathways for the elderly, linking hospitals, primary care centers, and geriatric day care facilities, with clearly defined roles, referral protocols, and shared health records. Potential barriers include weak enforcement mechanisms, limited intersectoral communication, and lack of infrastructure for shared health records. Addressing these will require phased implementation and strong leadership from the health ministry.
Poor performance of the Pension Fund in covering geriatric services
Participants highlighted the inadequate performance of the Pension Fund in supporting geriatric services. Kiani47 noted that pension organizations offer limited and declining support relative to the growing elderly population. Contributing factors include demographic shifts, economic instability, inflation, high unemployment, reduced inflow of new insurees, and increased retirees, all of which strain the funds and limit service coverage. One possible recommendation is to improve the sustainability of the Pension Fund by diversifying its funding sources and gradually expanding subsidies for essential geriatric services. However, financial constraints, political resistance to structural reform, and lack of long-term actuarial planning may hinder these efforts. Effective implementation will require cross-sector collaboration and strong economic forecasting.
Disregard for the personal and healthcare needs of the elderly
A key challenge identified was the neglect of elderly individuals’ personal and healthcare needs. Aging naturally brings new healthcare demands, yet these are often overlooked. Rafsanjani et al.48 found that elderly people in Rafsanjan lack adequate psychological and physical support, while Shariat et al.49 reported that Tehran’s elderly face unmet cultural, social, economic, and welfare needs. It is recommended that policymakers and managers develop comprehensive and participatory programs that address the individual, psychological, social, and cultural needs of the elderly, ensuring these aspects are not overlooked in health and welfare service planning. Yet, limited awareness, workforce shortages, and competing policy priorities may hinder program development and uptake. Tailored training and intersectoral advocacy are needed to overcome these barriers.
Failure to monitor the standards for GHCS provision
Safdari et al.50 noted that although some executive organizations in Iran attempt to support and monitor services for the elderly, these efforts are insufficient due to limited responsibilities and funding. Other studies have also cited the lack of standard care programs and their monitoring as key issues42. Ghamami et al.51 emphasized the need for targeted and regular monitoring with timely feedback. Additional challenges include lack of health-oriented and evidence-based policies, focus on treatment over prevention, and poor strategic planning38,41. These findings align with previous research highlighting weak decision-making and poor evaluation of geriatric programs17,52,53,54. A recommended policy is to develop a centralized monitoring system with clear standards and adequate funding to ensure regular evaluation and improve the quality and coordination of geriatric health care services. However, limited financial resources, organizational resistance, and inadequate data infrastructure may impede the establishment of such a system. Overcoming these barriers requires political commitment and capacity-building within responsible agencies.
Failure in empowering the geriatric healthcare providers
Several studies have highlighted inadequate knowledge, poor attitudes, and insufficient training among healthcare providers regarding geriatric care as key challenges55. The Iranian health system needs to recruit qualified geriatric specialists and enhance training for relevant personnel38. Poor nursing care quality has also been linked to limited education in this area44,56. A qualitative study recommended strategies such as specialized training courses, workshops, and incorporating geriatric topics into academic curricula57. Overall, limited expertise negatively affects the quality of care and calls for policy interventions by senior health authorities. The Ministry of Health should implement a national program to enhance geriatric care capacity through specialized training, curriculum integration, and systematic recruitment of geriatric specialists, in collaboration with relevant professional bodies. Nonetheless, challenges such as limited funding, resistance to curriculum changes, and shortages of qualified trainers may delay these initiatives. Strong leadership and stakeholder engagement are essential to address these obstacles effectively.
Poor medication management
Experts identified medication issues, including shortages and limited access, as key challenges in geriatric healthcare. Parsa noted that lack of insurance coverage limits elderly access to some medicines58, and Nascimento et al.59 highlighted medication access issues in geriatric care. To address these challenges, it is recommended that essential geriatric medications be included in the national drug list and fully covered by insurance. Establishing a centralized pharmaceutical database to monitor medication usage patterns and anticipate shortages can further enhance system responsiveness. In parallel, promoting rational prescribing practices through continuous provider education and the implementation of electronic prescription systems is essential. Moreover, providing essential medicines free of charge to low-income elderly individuals and improving accessibility through investment in domestic pharmaceutical production are also critical components of an effective national strategy.
Absence of a specific executive model for providing routine primary GHCSs
Another issue related to the provision of geriatric healthcare was the lack of a specific executive model for providing routine primary GHCSs. In this regard, Mohammadi-Shahboulagh et al.43 proposed a model for providing outpatient healthcare services to the elderly, believing that such models can lead to rapid diagnostics of health problems and timely intervention in the elderly, because implementing this model makes it possible to prevent diseases and their complications as well as the additional costs imposed on older adults and their family, as well as the health system. However, barriers such as limited infrastructure, insufficient trained personnel, and lack of clear operational guidelines may challenge the practical implementation of such models. Gradual piloting and resource allocation are recommended to facilitate adoption.
Elderly’s failure to complete the treatment program
A key challenge in GHCS provision is elderly patients’ non-adherence to medication or failure to complete treatment. Khodabandeh et al.44 attributed this to inadequate guidance from healthcare providers, while Zanganeh Baygi et al.60 cited factors such as financial hardship, limited access, distrust, drug interactions, and lack of motivation. Addressing this issue requires improving elderly health literacy, expanding insurance, offering financial/moral support, and enhancing access to medications and treatment centers. Nonetheless, barriers such as limited healthcare workforce time, systemic insurance constraints, and persistent social stigma may impede progress. Multisectoral efforts and patient-centered approaches are essential to overcome these challenges.
Lack of suitable places to provide GHCSs and other welfare facilities
A major challenge identified was the lack of appropriate spaces and welfare facilities for GHCSs. Studies have highlighted the absence of specialized geriatric clinics, dedicated service lines, and adequate facilities in medical centers37,41,44,45,56,61. The number of geriatric care beds in Iran is also significantly below international standards62. Other issues include overcrowded centers, poor-quality health environments43,46, and insufficient emotional, informational, and service support63. To address this, decision-makers should adapt healthcare settings by removing physical barriers, improving mobility, and upgrading equipment to meet elderly needs. However, limited financial resources, outdated infrastructure, and competing health system priorities may hinder the timely implementation of such improvements. Prioritizing high-need areas and leveraging public–private partnerships could help overcome these constraints.
Shortage/inappropriate distribution of geriatric specialists
The shortage or inappropriate distribution of geriatric specialists was another identified major challenge regarding geriatric health, which has been reported in various studies as well. Firoozeh38, Khodabandeh44 and Goharinezhad41 also considered the shortage/inappropriate distribution of geriatric specialists to be one of the main challenges in providing geriatric healthcare. To compensate for this shortage, Mohebi et al.57 proposed some strategies including using doctors for at least three days a week in healthcare centers and homes, and increasing the number of geriatric specialists by increasing the capacity of geriatric health disciplines and developing related disciplines, especially in less-developed areas. However, limited academic infrastructure, low motivation among medical graduates to specialize in geriatrics, and budgetary constraints may delay these efforts. Strategic incentives and targeted investment in training programs are needed to address these barriers.
Lack of a registry or database system for the elderly
Regarding the information challenge in GHCS provision, although the health information system is available in the geriatric health sector in Iran, it faces some challenges. The lack of electronic health records and consequently the lack of access to disease history, as well as the lack of an integrated information system for older adults, and the manual referral of this age group by health centers to more specialized centers were other challenges identified in the present study and reported in some previous studies37,41,50. Since a registry and database system is a requirement in monitoring and controlling health status and risky diseases and plays a major role in the systematic collection and optimal processing of health and disease-related data, it seems essential that MOHME take actions to develop and optimize this system in order to provide high-quality services to the elderly. Nevertheless, potential barriers such as fragmented data systems, limited digital infrastructure in rural areas, and concerns about data privacy may hinder implementation. Ensuring interoperability and allocating dedicated IT resources are crucial steps for overcoming these challenges.
Lack of a unified organization and inadequate authority of healthcare professionals to provide geriatric services
Another important identified challenge regarding GHCS provision in Iran was the lack of a unified organization with adequate authority as the custodian of geriatric services. In this regard, Safdari50 and Firoozeh38 discussed the lack of a specific custodian of geriatric health and the inactivity of the National Council on Geriatric Health. This challenge is distinct from inter-organizational coordination, as it focuses on the structural absence of a single authoritative body within the Ministry of Health with clear stewardship over GHCSs. Some other studies also assessed the poor intersectoral collaboration between the main stakeholders of geriatric health37,38,39,41,44,50. Therefore, it seems essential to set up a department with a clear organizational structure and level of responsibility and authority in MOHME to address the geriatric healthcare system, so that it can more effectively oversee the HCSs provided to the elderly. However, potential barriers may include institutional resistance to restructuring, overlapping mandates with existing departments, and limited budgetary or political support. Building consensus among stakeholders and clearly defining the new department’s authority will be crucial for successful implementation.
Non-implementation of national policy document on ageing (NPDA) provisions
Participants identified the poor implementation of the NPDA in Iran, approved in 2019, as a key challenge. Although the NPDA outlined six main goals—ranging from elderly empowerment to financial support—experts noted it has not been effectively executed. Goodarzi et al.64 attributed this to weak laws and regulations and emphasized the need for a dedicated custodian, stronger enforcement, and reform of inefficient or burdensome laws. The government should designate a lead agency to oversee and coordinate the implementation of the NPDA, strengthen legal frameworks for enforcement, and reform ineffective regulations to ensure the policy’s goals are translated into actionable programs. However, this requires overcoming potential barriers such as limited intersectoral commitment, bureaucratic inertia, and lack of political will, which may hinder effective coordination and enforcement.
Lack of educational and communicative programs tailored to the needs of the elderly
Another identified challenge regarding GHCS provision was the low knowledge and unawareness of the elderly. In this regard, Parsa et al.58 pointed out this age group’s low knowledge regarding medication use, which aggravated their problems in this regard. Therefore, training, empowerment and appropriate interventions to improve the seniors’ level of knowledge and awareness about healthcare and medications seem necessary. In this regard, the capacity of the elderly’s families can also be utilized. However, developing such programs may face challenges such as limited geriatric-friendly educational materials, low digital literacy among older adults, and inadequate training for healthcare educators.
Unequal distribution of services
A key challenge highlighted by experts was the unequal distribution of GHCSs. Tajvar et al.65 reported that seniors with higher socioeconomic status benefit more from HCSs, indicating disparities in access. Other studies have noted the concentration of services in metropolitan areas and uneven access within cities based on income levels37,41,44,45. The Ministry of Health should adopt a needs-based allocation model to ensure equitable distribution of geriatric health care services, prioritizing underserved regions and low-income populations through targeted resource allocation and service expansion. Nonetheless, achieving equitable service distribution may be constrained by resource limitations, local workforce shortages, and resistance to reallocating funds from urban centers to rural or deprived areas.
link